34 MENOPAUSE SYMPTOMS |
HEALTH CENTER |
|
| |
|
|
|
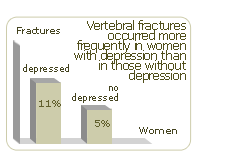
Women with depression were at increased risk for falls and fractures |
A recent research made by the team of researchers from the San Francisco Veterans Affairs Medical Center, UCSF, the University of Pittsburgh and the University of Minnesota at Minneapolis, reveal that older women with depression face an increased risk of fracture over their non-depressed counterparts.
|
|
Previous studies have suggested that depression is associated with low bone mineral density, and it is widely accepted that low bone mineral density leads to weaker bones. Until now, nevertheless, depression was never directly associated to an increased risk of fracture.
The investigators conducted a prospective research in elderly white women who were recruited from population-based listings in the United States. At a second visit (1988-1990), 7414 subjects completed the 15-item Geriatric Depression Scale and were considered depressed if they reported 6 or more symptoms of depression. The investigators measured bone mineral density (BMD) in the spine and at the second visit, asked participants about incident falls (yes/no) at 4 follow-up visits. Nonvertebral fracture were ascertained for an average of 6 years following the depression measure, and verified radiologically. We determined incident vertebral fractures by comparing lateral spine films obtained at the first visit (1986-1988) with repeat films got an average of 3.7 years |
|
Paradoxical to earlier findings, the study revealed no differences in average bone mineral density between depressed and non-depressed women. Even without a difference in bone density, nonetheless, depressed women were at greater risk for fracture. "This study highlights the severe disabilities associated with depression," said principal investigator Mary A. Whooley, SFVAMC staff physician and UCSF assistant professor of medicine. "Better diagnosis and treatment of depression may lead to decreased fracture", she added. |
 |
|
Poor diet is a well-known contributory factor to osteoporosis, or brittle bone disease, in later life. But it is possible, as other studies have suggested, that increased levels of the hormone produced by stress, cortisol, could adversely affect bone tissue.
Over three years, 329 of them suffered a hip fracture, and they were all asked questions relating to loneliness, life satisfaction, sleep disorders, anxiety and general mood.
Traditional factors known to increase the risk that falling will breaka hip, such as body weight, smoking, inactivity and other illness were taken into account.
Elderly people are falling down like ninepins, but injury/ rates are quite low, in terms of actually getting serious injury like a broken hip. It is possible that depressed people are not looking after their diet as well, and this is contributing to osteoporosis."
The study concluded that depression is a significant risk factor for fracture in older women. The greater frequency of falls among individuals with depression partially explains this finding. Other mechanisms responsible for the association between depression and fracture remain to be determined.
By Natural-Progesterone-Estrogen-Supplements.com |
 |
|
|
|
|
| |
Copyright� 2008 - - All Rights Reserved |
|
|


